FAQ on the West Nile virus
Disclaimer
The contents of this website are for general information purposes only and do not constitute medical advice, diagnosis or treatment. They are not a substitute for individual consultation with a qualified medical professional.
No guarantee is given for the accuracy, completeness or timeliness of the information provided. Use of the content is at your own risk. If you have any health questions or complaints, please always consult a doctor or other qualified professional.
1. What is the West Nile virus?
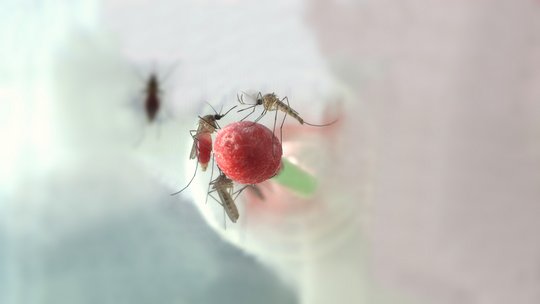
The West Nile virus (WNV), scientifically known as Orthoflavivirus nilense, is a virus from the Flaviviridae family. It was first isolated in 1937 in the West Nile district of Uganda, but is now found in many parts of the world, including Europe and Germany. The virus is mainly transmitted by mosquitoes and can cause West Nile fever in humans.
2. How is the West Nile virus transmitted?
West Nile virus is transmitted by the bite of infected mosquitoes, primarily domestic mosquitoes of the species Culexpipiens (common mosquito) and related species of the Culex genus.
The natural transmission cycle occurs between birds and mosquitoes: mosquitoes become infected when they suck blood from infected birds and can then pass on the virus.
Humans and horses are considered dead-end hosts. In these hosts, the virus concentration in the blood (viremia) does not usually reach the threshold required for absorption by mosquitoes and further transmission. They can become ill, but do not usually play a role in the further spread of the virus.
There is no direct transmission from person to person. In very rare cases, the virus can be transmitted via blood transfusions or organ transplants. For this reason, targeted safety measures and blood donation testing are in place in Germany during the mosquito season.
3. Where does the West Nile virus occur?
The West Nile virus is widespread worldwide, including in Africa, North America, the Mediterranean region, and large parts of Europe.
In Germany, the virus was first detected in animals in 2018, followed by the first autochthonous human infections in subsequent years. Initially, this mainly affected birds and horses, but locally acquired infections in humans have now also been reported. Berlin, Brandenburg, Saxony, and Saxony-Anhalt, which are considered permanent transmission hubs, have been particularly affected so far. There have also been isolated cases in Schleswig-Holstein, Lower Saxony, Bavaria, and North Rhine-Westphalia. Regions in eastern and southeastern Germany have been particularly affected so far. In principle, however, the virus can occur anywhere where suitable mosquitoes are present.
The Paul Ehrlich Institute currently states that the transmission season in Germany is from June to November. Warm summers favor the virus's reproduction in mosquitoes and increase the risk of transmission.
4. What are the symptoms of West Nile virus infection?
About 80 percent of all infections are asymptomatic. Around 20 percent of those infected develop what is known as West Nile fever. In less than one percent of cases, a severe neuroinvasive disease develops.
If symptoms occur, they usually begin 2 to 14 days after the mosquito bite. Typical symptoms are:
- Fever
- Headache and body aches
- Fatigue and general feeling of illness
- Occasional skin rash or swollen lymph nodes
In rare cases, the virus can attack the nervous system. This can lead to meningitis or encephalitis. Possible signs include severe headache, neck stiffness, confusion, or paralysis.
Severe cases mainly affect older people and those with weakened immune systems or certain pre-existing conditions.
5. How is West Nile virus infection diagnosed?
In the early stages of the disease, the virus can be detected directly in the blood, for example using PCR.
After a few days, the body forms antibodies. Antibody tests (IgM/IgG) are then used. Since the symptoms are similar to those of other mosquito-borne diseases, laboratory diagnosis is important.
Cross-reactions with related flaviviruses, especially the Usutu virus (USUV), the TBE virus, and dengue viruses, pose a particular diagnostic challenge. Neutralization tests and, if necessary, metagenomic sequencing (mNGS) are used for reliable differentiation.
6. How is West Nile fever treated?
There is no specific antiviral therapy for West Nile virus. Treatment is symptomatic and depends on the symptoms:
- Fever reduction
- painkillers
- adequate fluid intake
- physical rest
In severe neurological cases, treatment in hospital is necessary.
7. Is there a vaccine against West Nile virus?
There is currently no approved vaccine against West Nile virus for humans.
Several vaccines are approved for horses in the EU. They are particularly recommended in endemic areas.
Researchers are working on vaccine candidates for humans, but these have not yet been approved.
8. What is the significance of West Nile virus for blood transfusions?
In rare cases, West Nile virus can be transmitted through blood transfusions. This risk is particularly high if an infected person has no or only very mild symptoms and donates blood during this phase.
In Germany, the Paul Ehrlich Institute stipulates that during the transmission season, all relevant blood donations must be tested for West Nile virus using nucleic acid amplification testing (NAT) (Section 28 of the German Medicines Act). Blood donation services test approximately 2.0 to 2.4 million donations for viral genetic material each year. This allows infections to be detected even if donors have no symptoms.
Alternatively, some blood donation services apply a temporary deferral procedure. People who have been in designated endemic areas are then not allowed to donate blood for a certain period of time. Both strategies help to reliably ensure the safety of the blood supply even when virus activity is increasing.
Current studies by the BNITM show that blood donors represent a kind of early warning system for monitoring the West Nile virus. Routine NAT screening detects infections even without symptoms. Supplementary genomic analyses make it possible to track transmission routes, virus evolution, and regional spread patterns.
9. How can you protect yourself against the West Nile virus?
The most important protection is to avoid mosquito bites, especially in the summer months:
- Use insect repellent on your skin and clothing.
- Wear light-colored, long-sleeved clothing and long pants.
- Use fly screens on windows and doors.
- Reduce potential mosquito breeding sites by avoiding standing water around the house.
People with an acute infection should avoid mosquito bites as much as possible to prevent further spread of the virus.
10. What role does climate change play?
Higher temperatures accelerate the mosquitoes' reproduction cycle and, above all, virus replication in the vector. This shortens the so-called extrinsic incubation period and increases the probability of transmission. In addition, longer periods of warm weather can lead to an extension of the transmission season. Experts therefore assume that the virus will continue to play an increasingly important role in Central Europe in the future.
11. What research is the BNITM conducting on the West Nile virus?
At the Bernhard Nocht Institute for Tropical Medicine, the West Nile virus is being researched from two complementary perspectives:
Vector competence and ecology: One focus is on how efficiently native mosquitoes can transmit WNV and which factors, including temperature, environmental conditions, and insect-specific viruses, influence the risk of transmission.
Genomic surveillance and diagnostics: Another focus is the genomic surveillance of WNV in Germany. Using state-of-the-art sequencing technologies, including metagenomic analysis (mNGS) and highly sensitive amplicon-based protocols, transmission routes are tracked, virus variants are characterized, and spread patterns are reconstructed. A particular focus is on the use of blood donor screening as an early warning system.
More information
Contact persons at BNITM
Dr. Renke Lühken
Mosquitoes, arbovirus ecology, vector competence
Dr. Dániel Cadar
Genomic surveillance, virus metagenomics and evolution, diagnostics, blood transfusion safety
Original publications
Stephanie Jansen et al.: Culex torrentium: A Potent Vector for the Transmission of West Nile Virus in Central Europe. Viruses 2019, 11(6), 492; doi.org/10.3390/v11060492
Stefano Orru et al.: Assessment of the effectiveness of West Nile virus screening by analysing suspected positive donations among blood donors, Germany, 2020 to 2023. Eurosurveillance Volume 30, Issue 8, 27/Feb/2025. doi.org/10.2807/1560-7917.ES.2025.30.8.2400373
Gábor Endre Tóth et al.: Blood donors as sentinels for genomic surveillance of West Nile virus in Germany using a sensitive amplicon-based sequencing approach. Viruses and Viral DiseasesVolume 91, Issue 5106647November 2025. doi.org/10.1016/j.jinf.2025.106647
- Dr Dániel Cadar
- Head of RG Virus Metagenomics and Evolution
- phone: +49 40 285380-840
- fax: +49 40 285380-400
- email: cadar@bnitm.de
- Dr Renke Lühken
- Group Leader Arbovirology Ecology
- phone: +49 40 285380-862
- email: luehken@bnitm.de
- BNITM Press
- phone: +49 40 285380-264/269
- email: presse@bnitm.de
- The Laboratory diagnostics|Consultation for physicians
- Advice on the diagnostic procedure
- phone: +49 40 285380-211
- fax: +49 40 285380-252
- email: labordiagnostik@bnitm.de






