
Encephalitides caused by bornaviruses (BoDV-1 and VSBV-1)
In 2018, human infections with the classic Borna disease virus 1 (BoDV-1) were described without doubt for the first time. These were severe encephalitides (brain infections). A few cases were acquired through transplantation; in the case of the other, sporadic infections, the exact route of infection is unclear. More than 40 such individual human infections are now known, most of them with fatal outcomes. Since 2020, there has been a laboratory diagnostic reporting obligation for the direct detection of the pathogen in humans; most cases have so far been reported from Bavaria.
BoDV-1 occurs naturally in field shrews (Crocidura leucodon), small mammals related to hedgehogs and moles. Endemic areas are Bavaria, Baden-Württemberg (north-east), Brandenburg, Saxony-Anhalt, Saxony (west) and Thuringia, but also areas of Austria, Liechtenstein and Switzerland. The virus has long been known to cause Borna's disease in horses and sheep in these areas.

In 2015, after the occurrence of fatal encephalitides in three private keepers of exotic variegated squirrels (Sciurus variegatoides) in Saxony-Anhalt, a novel bornavirus was discovered in Germany (variegated squirrel bornavirus 1; VSBV-1) following extensive molecular biological investigations of the patients and a variegated squirrel. Scratches and bites of the animals may be the route of infection. In addition to variegated squirrels, the virus has also been found in other exotic tree squirrels such as red-tailed squirrels (Sciurus granatensis), Finlayson squirrels (Callosciurus finlaysonii), Chinese tree chipmunks (Tamiops swinhoei) and especially Prevost's chipmunks (Callosciurus prevostii) in various private homes and zoos. The virus has not yet been detected in domestic squirrels. One death and one severe case of disease caused by VSBV-1 in animal keepers who had professional contact with squirrels have been detected in the meantime.

Laboratory diagnostics
Diagnostic methods are available at the Bernhard Nocht Institute for Tropical Medicine in Hamburg for acute encephalitis caused by BoDV-1 and VSBV-1. In particular, cases with severe encephalitis from the known endemic areas or stay in the endemic areas or after contact with exotic tree squirrels should be investigated:
- real time PCRs from cerebrospinal fluid and brain tissue
- antibody detection from serum and CSF (IIFT, immunoblot, ELISA).
Antibody detection in serum is currently the most sensitive detection method; Borna-specific antibodies appear later in CSF and are lower in titre. Virus RNA detection in CSF is usually only successful in earlier phases of the disease, but regularly in biopsies from inflamed areas. In the positive case, viral whole genome sequencing is performed using NGS to assign the isolate to a geographical cluster.
- in situ hybridisation and immunohistology can be performed from brain tissue.
Medical practices, clinics and institutes can also send serum, cerebrospinal fluid or brain tissue from encephalitis cases with an unclear diagnosis for retrospective examination. In particular, there is also the possibility of examining formalin-fixed archival samples embedded in paraffin.
Furthermore, patients with unclear neurological clinical pictures, household members of BoDV-1 and VSBV-1 patients, keepers of exotic tree squirrels and their household members and personnel from zoological gardens keeping exotic squirrels can be serologically tested.
Please use our examination order (only in German) to request the test.
Further information on the diagnostic procedure (tests, procedure, case definition; in English) can be found here in this publication and also in this publication. Further information on the background and our research can be found in the research projects of the research group Zoonoses.
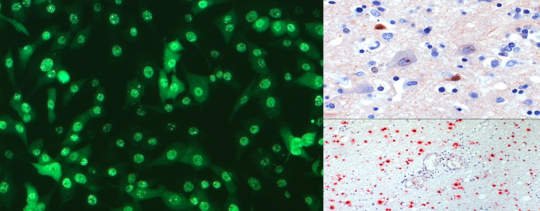
Clinic, imaging, cerebrospinal fluid and tissue findings
After a presumedincubationperiod of 3-4 months, both forms of bornavirus encephalitis present with febrile general symptoms with headache and change of character as well as cognitive slowing. This is often followed by myoclonia, bulbar deviations, ataxia, epileptic seizures, tetraparesis and coma as an expression of severe panencephalitis. Meningeal involvement may be present, as well as peripheral nervous system involvement, for example in the form of Guillain-Barré-like symptoms. In the vast majority of cases, the disease leads to death within about one to four months after the first symptoms appear; VSBV-1 encephalitis seems to have a slower course than infections caused by BoDV-1.
Abnormalities in the MRI can show up late, often only after about 2 weeks. In many cases, there is an affection of the basal ganglia (especially the caudate nerve) and the limbic system, with a differential diagnosis of seronegative autoimmune encephalitis. The CSF shows low to moderate lymphocytic pleocytosis, with markedly elevated protein and lactate concentrations. However, this constellation could also be different in individual cases. Histopathologically, a pronounced perivascular CD20+ and CD3+ lymphocytic infiltrate ("lymphocyte cuffing") is present, which can appear like a vasculitis. There is also marked microglial and astrocyte activation. Bornaviruses are not cytolytic, the severe tissue destruction is caused by immunopathogenesis.
Transmission, prevention and therapy
Field shrews infected with BoDV-1 and exotic squirrels infected with VSBV-1 appear healthy and show no conspicuous organ changes. However, they excrete the viruses with saliva and urine. Scratch or bite injuries as well as mucosal contact with virus-containing excretions of the animals are therefore possible routes of infection.
Direct contact with shrews and exotic squirrels as well as their carcasses and excretions should be avoided urgently. According to current knowledge, there is no transmission from human to human. Further information on BoDV-1 can be found here in the leaflet (only in German).
There is no established therapy. Ribavirin and especially favipiravir show inhibitory properties against bornaviruses in vitro; use in human infections is therefore conceivable. Whether an additional immunosuppressive therapy, which may possibly lead to longer survival, is useful can be discussed in view of the immunopathogenetic changes in bornavirus encephalitis.

Contact
Management
- Prof. Dr Dennis Tappe
- phone: +49 40 285380-499
- fax: +49 40 285380-252
- email: tappe@bnitm.de
Consultation for physicians only
Patients should contact their attending physician's office.
Consultation on diagnostic procedure
Physician
mo – fri 09:00 – 12:00 and 13:00 – 17:00
phone: +49 40 285380-211
fax: +49 40 285380-252
email: labordiagnostik@bnitm.de
Medical management
Prof. Dr Stephan Günther
Prof. Dr Dennis Tappe
Specialists in Microbiology, Virology & Infectious Disease Epidemiology
Probenversand an
Bernhard-Nocht-Institut für Tropenmedizin
Zentrale Labordiagnostik
Bernhard-Nocht-Straße 74
20359 Hamburg






