Hidden infections, new outbreaks
Why mobility matters when Ebola returns
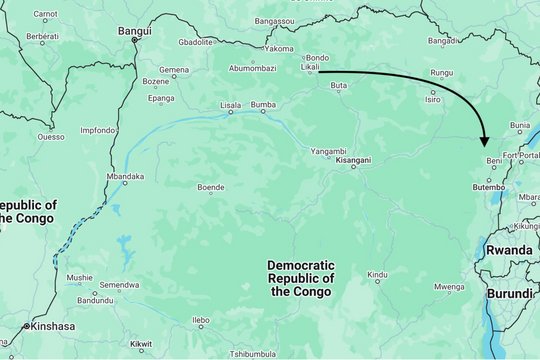
A man climbs onto a motorbike. Behind him lies a remote forest area in the Likati region in the north of the Democratic Republic of Congo (DR Congo). Ahead of him is a journey of almost 900 kilometres to the gold mines in the east of the country. He travels along damaged roads, then switches to a truck, before finally continuing on foot. At the gold mines, he meets many people. A few months later, one of the largest Ebola outbreaks in history begins in the wider area. What sounds like a coincidence could be a crucial clue: Researchers at the Bernhard Nocht Institute for Tropical Medicine (BNITM) have collaborated with partners in the DR Congo to investigate whether the 2017 Likati and 2018-2020 Ituri/North Kivu Ebola outbreaks could be linked by the mobility of survivors. The results were published in the journal BMC Infectious Diseases.

Ebola is considered to be highly dangerous but rare. The disease caused by the Ebola virus usually has a sudden onset of high fever and can lead to severe organ failure and internal bleeding. If left untreated, the infectious disease is often fatal. The virus repeatedly causes outbreaks in the DR Congo. Interestingly, Ebola outbreaks there do not occur randomly, but certain regions repeatedly emerge as hotspots. The 2018-2020 outbreak in Ituri and North Kivu was the second largest in the world. A total of 3,470 cases were confirmed, with 2,287 deaths. Genetic analyses of the virus showed that this outbreak could be linked to a smaller, earlier outbreak in Likati in 2017. But how can an outbreak in a remote forest area be linked to a later outbreak in the east of the country?
This is where Sung Joon Park, head of the Medical Anthropology Research Group at BNITM, and his team come in. Rather than examining laboratory data alone, the researchers combine epidemiological analysis with social science fieldwork. In this study, the research team explored a hypothesis that had long been underestimated: the Ebola virus can persist for years in the bodily fluids of survivors without them showing any symptoms of the disease. As a result, survivors could unknowingly trigger new chains of infection months or even years after an outbreak – and not only at the original site of the Ebola outbreak: when they travel, the viruses may travel with them.
But who actually travels? Who leaves their village and who stays? Which routes are possible and which are not? In the DR Congo, mobility is not just a question of distance.
"Mobility depends on whether someone has money and contacts, whether transport and passable roads are available, and whether they have the physical strength for a long journey. These factors can determine whether a virus stays in one place or spreads to another region. 900 kilometres on a map may look like a straight line, but in reality it is a journey through social and infrastructural boundaries," explains Park, first author of the study.

Medical anthropology as detective work
Between April 2022 and May 2023, the research team conducted a retrospective transdisciplinary study, combining various scientific disciplines and methods (including interviews and molecular analyses). Using a snowball method, they spoke to survivors and contact persons, asking them to name others who had left Likati after the outbreak. In several affected villages, they conducted open and semi-structured interviews and moderated group discussions.

In addition, they accompanied people on their journeys to understand mobility not only through interviews, but also in praxis. At the same time, they examined blood and semen samples using modern laboratory methods. They used an antibody test to determine whether a person had previously been infected with Ebola. Additionally, the team tested semen samples for Ebola virus RNA, as it is known that Ebola viruses can survive for long periods in certain bodily fluids.
"This approach exemplifies how medical anthropology works. It reconstructs social realities, movement patterns and living conditions, revealing what often remains invisible in traditional surveillance systems," says Park.
A survivor who was not officially one
The decisive clue led to a man who had been in close contact with Ebola patients in 2017. He had helped to transport a seriously ill patient on his motorbike. The man himself was not tested at the time. He later reported that he had experienced no typical symptoms, only severe fatigue. This is what makes the case so special: The research team suspected that he had survived Ebola without being registered as a survivor. After the outbreak, he travelled to a gold mining area in Badengayido in Ituri province. This area is located approximately180 kilometres west of Mangina, where the first cases of the major 2018-2020 Ebola outbreak were later reported.
Laboratory analyses confirmed the researchers' suspicion. An antibody test clearly showed that the man had been infected with Ebola virus. The team thus identified an Ebola survivor who was not officially recognised as such. Testing the semen sample for Ebola virus RNA yielded a negative result. This means that no virus was detected in this sample. Nevertheless, the case remains epidemiologically significant, as the man travelled at a critical time to an area that was later severely affected by the outbreak.
A possible scenario – implications for future outbreaks
The researchers found no evidence that any other survivors or contacts from Likati had travelled east before the 2018 outbreak. This left the man as the only known case who had both close contact with Ebola patients and travelled to the area at the critical time before the outbreak. While the study does not provide definitive proof that the major 2018-2020 Ebola outbreak actually originated from the Likati outbreak, it presents a plausible scenario that is easily overlooked in classic epidemiological analyses. At the same time, it highlights the importance of asymptomatic or mild cases. Such cases may occur more frequently than previously assumed and would go undetected in many outbreak situations. As a result, these individuals would also not be included in prevention measures.
"This case shows how quickly people can disappear from the radar of official systems," says Park. "If someone is not tested, they do not appear in any statistics. But they remain part of the epidemiological reality. A person who does not see themselves as a survivor will receive no counselling, no follow-up care and no information about potential long-term risks."
The researchers therefore emphasise the need for robust follow-up systems after Ebola outbreaks, even for people without apparent symptoms. It is particularly important to provide long-term support to survivors. Improved methods could help track the mobility of survivors and better integrate it into surveillance strategies. Mobile health units could also help to provide regular care for survivors in remote regions and detect possible new infections early.
"Our study shows that outbreak control is not determined in the laboratory alone. It also requires field research, local perspectives, and an understanding of how people actually live. Medical anthropology therefore makes a concrete contribution to global health research," Park concludes.

Publication:
Park, S.J. et al. Investigating the spatiotemporal links between the EVD outbreaks in Likati (2017) and Eastern DRC (2018–2020): a retrospective transdisciplinary study. BMC Infect Dis (2026). DOI: 10.1186/s12879-026-12607-0
Cooperations:
Institut National de Recherche Biomédicale, INRB, Kinshasa, Democratic Republic of the Congo
University of Kinshasa, Kinshasa, Democratic Republic of the Congo
Rodolphe Mérieux INRB-Goma Laboratory, Goma, North-Kivu, Democratic Republic of the Congo
Pole Institute Goma, Goma, North-Kivu, Democratic Republic of the Congo
Contact person
Dr Sung-Joon (Song) Park
Leader RG Medical Anthropology
Phone : +49 40 285380 711
Email : sung.park@bnitm.de
Dr Anna Hein
Public Relations
Phone : +49 40 285380-269
Email : presse@bnitm.de
Further information






